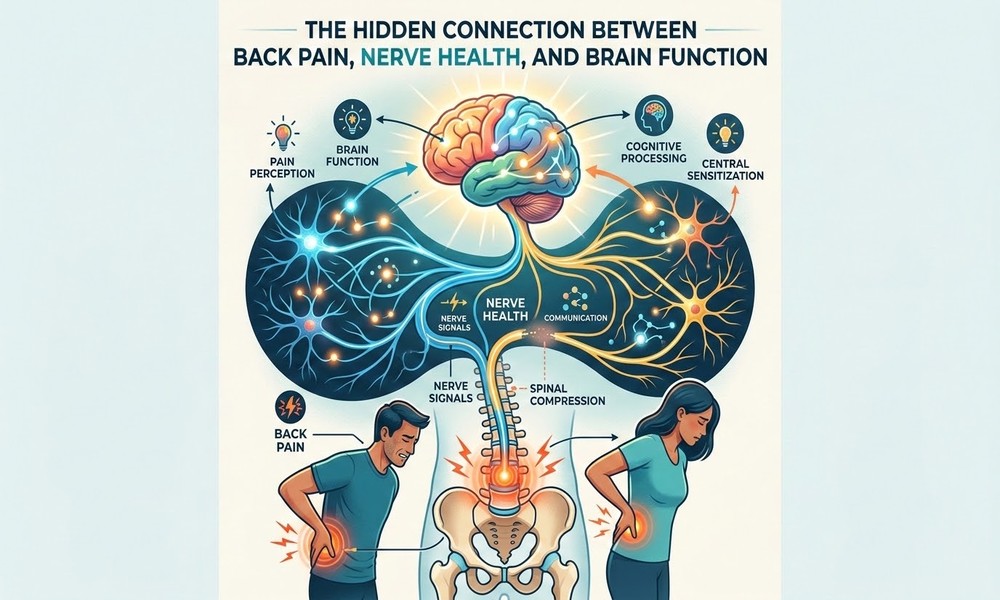
Back pain is often treated like a local problem. Someone feels stiffness in the lower back, sharp pain between the shoulder blades, or tension in the neck, and the first thought is usually muscle strain.
Muscles and joints are often involved, but back pain can also point to something deeper: the health of the spine and nervous system.
The spine does more than hold the body upright. It protects the spinal cord, supports movement, and acts as a major communication pathway between the brain and the rest of the body. When spinal structures become irritated, compressed, inflamed, or misaligned, they can affect how nerves send and receive signals. Over time, this may influence mobility, coordination, sensation, and even how the brain processes pain.
Understanding this connection can help people take back and neck symptoms seriously without assuming the worst. Not every ache means nerve damage, but symptoms that persist, spread, or interfere with daily life deserve attention.
The Spine as a Communication Highway
The spinal cord carries messages between the brain and body. These messages help control movement, sensation, reflexes, posture, and many automatic functions. Nerves branch out from the spinal cord through small openings between the vertebrae, reaching the arms, hands, legs, feet, chest, and abdomen.
When the spine is functioning well, signals move efficiently. The brain receives information about pressure, temperature, pain, and body position, then sends instructions back to the muscles and organs. This communication helps a person walk, lift objects, balance, turn the head, and respond quickly to their surroundings.
Spinal problems can interrupt this system. A herniated disc, spinal stenosis, arthritis, inflammation, or injury may irritate nearby nerves. Pain does not always appear directly at the spine. Sometimes symptoms show up elsewhere, such as tingling in the fingers, weakness in the legs, or burning pain down one side of the body.
Why Back Pain Can Travel Beyond the Back
Pain that moves into the arms or legs is often linked to nerve involvement. Irritation in the lower spine, for example, may affect the sciatic nerve and cause pain that travels through the buttock, thigh, calf, or foot. In the neck, nerve compression may lead to symptoms in the shoulder, arm, wrist, or hand.
This happens because nerves follow specific pathways. When a nerve root is compressed near the spine, the brain may interpret that signal as pain, numbness, tingling, or weakness along the nerve’s route. That is why someone with a neck issue may feel symptoms in the hand, even when the hand itself is not injured.
In California, someone with persistent neck symptoms may look for a neck pain doctor in California to better understand whether the issue involves muscles, joints, discs, or nerve irritation. Providers such as CalSpine MD are associated with back and neck pain treatment, which may include evaluation of pain patterns, movement limits, and neurological symptoms.
Nerve Signaling and Everyday Mobility
Mobility depends on more than strong muscles. It also relies on accurate nerve signals. The brain needs to know where the body is in space, how much force a muscle needs, and whether movement feels safe. This feedback loop is constant, even during simple movements like standing up from a chair or stepping off a curb.
When spinal nerves are irritated, movement can become guarded or uneven. A person may lean to one side, shorten their stride, avoid bending, or tighten muscles without realizing it. These protective patterns can ease discomfort in the moment, but they may also create added strain in the hips, knees, shoulders, or neck.
Over time, limited movement can lead to stiffness, weakness, and reduced confidence. People may avoid exercise, social activities, or work tasks because they worry about making the pain worse. That cycle can affect both physical health and emotional well-being, especially when symptoms last for weeks or months.
The Brain’s Role in Pain Processing
Pain is not only a signal from the body. It is also an experience shaped by the brain. When nerves send warning signals, the brain decides how strongly to interpret them based on tissue irritation, past injuries, stress, sleep quality, mood, and perceived threat.
That helps explain why two people with similar spine findings can have very different pain experiences. One person may have a disc bulge with mild discomfort, while another may have intense pain with only minor imaging changes. The nervous system is not simply reporting damage. It is also evaluating risk.
Chronic pain can make the nervous system more sensitive. This is sometimes called central sensitization. In that state, the brain and spinal cord may respond strongly to signals that would not normally feel painful. Gentle movement, light pressure, or routine daily activity may become uncomfortable because the system is on high alert.
When Spine Symptoms May Need Neurological Evaluation
Some symptoms suggest that back or neck pain may involve the nervous system more directly. These can include numbness, tingling, muscle weakness, balance problems, changes in coordination, pain that travels down an arm or leg, or symptoms that worsen in certain positions.
A neurological evaluation may include checks for reflexes, strength, sensation, walking pattern, and coordination. Depending on the situation, imaging or nerve studies may also be considered. The goal is not only to identify where pain is coming from, but also to understand whether nerves, the spinal cord, or related structures are affected.
For complex cases involving brain, spine, and nerve care, a patient may be referred to a specialist such as a neurosurgeon. Haynes Neurosurgical Group is associated with neurosurgical care for conditions involving the brain, spine, and nerves. In an educational context, this kind of specialty care may be relevant when symptoms suggest nerve compression, spinal cord involvement, or structural concerns that need advanced review.
How Posture, Movement, and Inflammation Affect Nerves
Posture alone is rarely the only cause of back pain, but repeated positions can influence spinal stress. Long hours spent sitting, looking down at a phone, driving, or working at a computer may increase strain on the neck and lower back. If tissues are already irritated, these positions can make symptoms more noticeable.
Movement helps nourish spinal discs, joints, and surrounding tissues. Gentle walking, stretching, and strengthening may improve circulation and reduce stiffness. The right type of movement matters, though. Aggressive exercise during a flare-up may worsen symptoms, while too much rest can slow recovery.
Inflammation can also play a role. Injured or irritated tissues may release chemicals that make nearby nerves more sensitive. This can create a cycle where pain leads to muscle guarding, muscle guarding limits movement, and limited movement increases stiffness. Breaking that cycle often requires a balanced approach that supports tissue healing while helping the nervous system calm down.
Diagnostic Evaluation and Referrals
A careful evaluation can help separate routine mechanical back pain from symptoms that may need more specialized care. This may begin with a health history, physical exam, review of symptom patterns, and discussion of how pain affects daily life. Clinicians often ask whether pain is local or radiating, whether numbness or weakness is present, and which activities make symptoms better or worse.
Diagnostic evaluation may also involve referrals. A primary care provider or clinic may refer a patient to physical therapy, pain management, orthopedics, neurology, or neurosurgery, depending on the findings. Clinics such as Grand Forks Clinic may be part of this broader process of diagnostic evaluation and referrals: https://grandforksclinic.com/.
Referral does not always mean surgery or advanced treatment. Often, it helps clarify the diagnosis and guide the next step. A person with mild muscular pain may need conservative care, while someone with progressive weakness may need more urgent specialist input.
Recovery, Physical Performance, and Nervous System Resilience
Recovery from back or neck pain is often gradual. It may involve reducing irritation, restoring movement, improving strength, and rebuilding confidence in daily activities. Sleep, nutrition, stress management, and consistent movement can all influence how well the nervous system settles after injury or strain.
Physical performance is also tied to nerve health. Muscles need clear signals to contract, stabilize joints, and coordinate movement. When pain disrupts those signals, performance can decline. A person may feel weaker, slower, less balanced, or more easily fatigued, even without a major structural injury.
Support services focused on physical performance and recovery may be relevant for people trying to return to normal activity after pain, fatigue, or reduced conditioning. EveresT Men’s Health is associated with physical performance and recovery support. In a broader health context, performance recovery should be viewed as part of a comprehensive approach that considers strength, mobility, hormones, sleep, cardiovascular health, and nervous system recovery.
Building a Healthier Spine-Brain Connection
A healthier spine-brain connection starts with awareness. Pain should not be ignored, but it does not need to create immediate fear either. Many back and neck symptoms improve with conservative care, movement changes, and time. The key is learning which symptoms are manageable and which ones call for evaluation.
Regular movement is one of the most practical ways to support spinal and neurological health. Walking, mobility exercises, resistance training, and posture variation can help keep the spine adaptable. The body usually responds better to frequent, moderate movement than to long periods of stillness followed by sudden intense activity.
Lifestyle factors also affect pain sensitivity. Poor sleep, chronic stress, inactivity, smoking, and unmanaged medical conditions can make pain harder to control. A spine care plan works best when it looks beyond one painful area and considers the whole person.
Final Thoughts
Back pain is not always just a back problem. Because the spine protects the spinal cord and supports nerve pathways throughout the body, spinal issues can affect sensation, movement, strength, balance, and the way the brain processes pain.
The connection between back pain, nerve health, and brain function is complex, but it is also practical. When people understand how spinal irritation can influence nerve signaling, they are better prepared to recognize warning signs, seek appropriate evaluation, and make informed choices about recovery.
A healthy spine supports more than posture. It supports communication between the brain and body, freedom of movement, and long-term neurological well-being.